Mouth sores that burn, sting, or bleed can make eating, drinking, and talking hard. If this started during chemotherapy or radiotherapy, or after repeated mouth irritation, it is normal to feel worried. Many people search because they want quick relief and to know if it is serious.
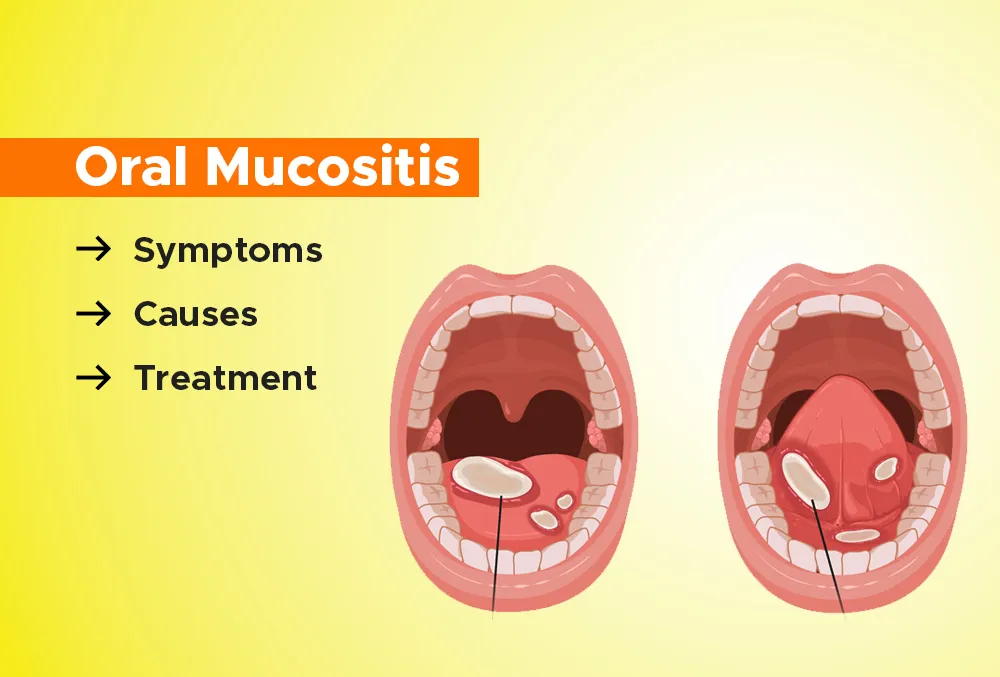
Oral mucositis is when the soft lining inside your mouth becomes inflamed and develops painful sores. It can cause redness, swelling, and ulcers, and it can also raise infection risk if it worsens.
At National Dental Care, we help you follow a clear path from oral mucositis symptoms to likely oral mucositis causes, and then the safest oral mucositis treatment steps. This includes an oral exam, identifying triggers like sharp teeth or denture irritation, and guiding supportive care to reduce pain and protect healing.
Read on to know what to do today and when to visit a dentist.
Understanding Oral Mucositis
Oral mucositis is when the soft skin lining the inside of the mouth becomes sore, inflamed, and breaks into painful areas or ulcers.
This lining is called the oral mucosa. When it becomes irritated, inflammation develops and healing slows. The condition may also be referred to as oral-mucositis or stomatitis, but mucositis usually describes deeper and more widespread soreness.
Which Parts Of The Mouth Are Affected?
Oral mucositis can appear on different areas inside the mouth, including –
- The tongue,
- The palate on the roof of the mouth,
- The buccal mucosa inside the cheeks,
- The gingiva or gums,
- Sometimes the oropharynx at the back of the throat.
How Oral Mucositis Is Different From Common Mouth Sores?
Oral mucositis usually lasts longer and causes more discomfort than a small, occasional mouth ulcer.
It often spreads across larger areas and forms multiple lesions. The underlying tissue is inflamed, which explains why the pain feels deeper and daily activities become harder.
How Do You Know If You Have Oral Mocositis?
Oral mucositis is likely when mouth soreness keeps increasing instead of improving within a few days.
Common Oral Mocositis Symptoms
- Pain, burning, soreness, and tenderness,
- Swelling and redness, sometimes with shiny gums,
- White patches or a pseudomembrane,
- Open ulcers and visible ulceration,
- Bleeding or pus in severe cases,
- Bad breath, also called halitosis,
- Difficulty eating,
- Difficulty swallowing, also called dysphagia,
- Difficulty talking,
- Thick saliva,
- Dry mouth, also called xerostomia,
- Bright redness known as erythema and puffiness called edema.
When pain increases, food and fluid intake often reduce. This can lead to dehydration, weight loss, low energy, and increased infection risk if not addressed early.
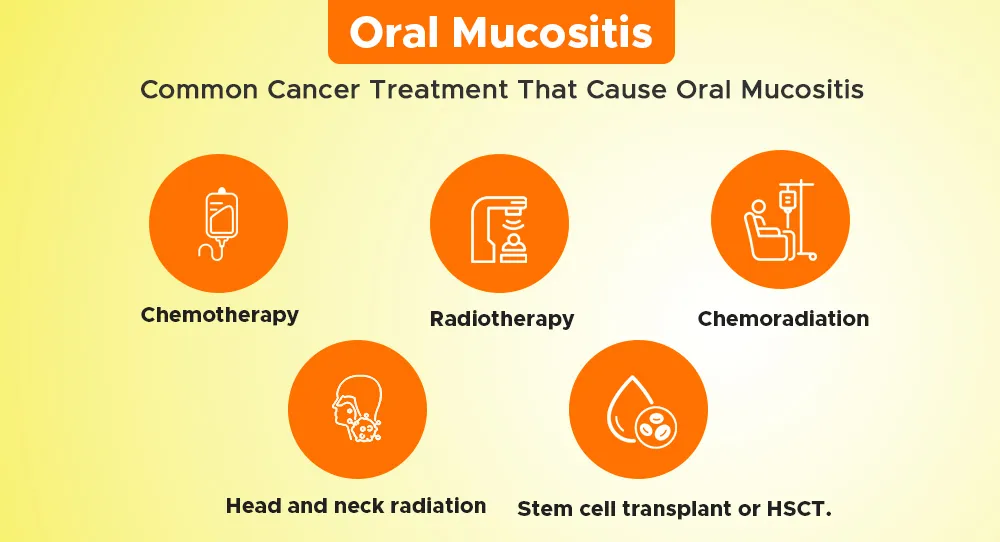
Why Does Oral Mucositis Happen During Cancer Treatment?
Cancer treatments affect fast-healing cells, including the lining inside the mouth.
Chemotherapy, radiotherapy, and related treatments slow healing and weaken the mouth’s natural protection. As a result, the oral mucosa becomes fragile and inflamed, allowing sores to form quickly.
Can Oral Mucositis Happen Without Cancer Treatment Too?
Yes. Oral mucositis can also develop due to repeated irritation, injury, infection, or nutritional gaps.
Common non-cancer causes include:
- Trauma from sharp teeth,
- Ill-fitting dentures,
- Burns from very hot food or drinks,
- Oral piercings,
- Poor oral hygiene,
- Infections such as candidiasis or HSV,
- Nutritional deficiency, including zinc deficiency.
These causes still need proper evaluation to prevent worsening or infection.
What Should You Do To Reduce Mouth Pain And Burning?
You can ease mouth pain and burning by protecting the sore areas and avoiding anything that irritates them further. Gentle care from the first day helps prevent sores from worsening.
Same Day Comfort Steps
- Maintain oral hygiene using a soft toothbrush,
- Rinse the mouth with a bland rinse like saline or sodium bicarbonate solution,
- Keep the mouth moist using a saliva substitute or artificial saliva,
- Apply a protective gel or mucosal coating if advised,
- Avoid spicy, acidic, rough, or very hot foods.
Short Term Pain Relief Options
- Use a topical anesthetic such as lidocaine only if prescribed,
- Follow magic mouthwash instructions carefully if given by your doctor,
- Use ice chips for short periods if recommended during treatment.
All these tips help reduce irritation, control pain, and support healing while you monitor symptoms.
Expert-Recommended, Safe 7 Day Routine for Oral Mucositis Care
| Time of Day | What to Do |
|---|---|
| Morning | Brush gently with a soft toothbrush and rinse with a bland solution like saline or sodium bicarbonate. |
| After meals | Rinse the mouth to clear food and reduce irritation on sore areas. |
| During the day | Sip water often to prevent dryness and keep the mouth comfortable. |
| Evening | Repeat gentle cleaning and apply any prescribed protective gel if advised. |
| Bedtime | Keep lips moisturised and avoid dry air while sleeping. |
Pain should gradually reduce and swallowing should feel easier. If symptoms worsen or fever appears, dental care should not be delayed.
What Treatments Are Used for Oral Mucositis Treatment?
Oral mucositis treatment focuses on reducing pain, preventing infection, and helping the mouth heal safely. The exact treatment depends on how severe the sores are and what caused them.
Supportive Treatments Commonly Used for Oral Mucositis
These are used in most mild to moderate cases:
- Pain relief medicines to control discomfort,
- Protective gels that coat sore areas and reduce irritation,
- Saliva substitutes to ease dryness and improve comfort,
- Bland mouth rinses to keep the mouth clean without stinging,
- Ice chips in selected cases during chemotherapy to reduce sore formation.
Medicines Used When Oral Mucositis Symptoms Are Severe
If pain or infection risk increases, doctors may prescribe:
- Antifungal medicines if yeast infection is present,
- Antiviral medicines for viral causes,
- Antibiotics if bacterial infection develops,
- Stronger pain medicines when simple options are not enough,
- Nutritional supplements if eating becomes difficult.
Signs You Need Urgent Help for Oral Mucositis
You should seek urgent help if mouth sores stop you from eating or drinking, or if signs of infection start to appear. Warning signs that you must not ignore includes –
- You cannot drink fluids for 24 hours,
- Pain keeps getting worse despite home care,
- Fever develops or you feel unusually weak,
- Pus or heavy bleeding appears from sores,
- Mouth ulcers spread quickly or look infected.
Dental Treatment for Mouth Sores
When you plan to visit a dental clinic for mouth sores, the dentist will carefully examine the sore areas inside your mouth to understand what is causing the pain. They look at the location, size, and severity of the sores and check whether the surrounding tissue is inflamed or infected.
What Problems Dentists Rule Out During the Visit?
Here’s what the dentists check during the visit for mouth sores.
- Sharp teeth or rough edges causing repeated injury,
- Ill fitting dentures or appliances,
- Signs of fungal or viral infection,
- Excess dryness or saliva changes,
- Gum or tissue damage that needs protection.
Based on what is found, the dentist suggests steps to reduce pain, protect healing tissue, and prevent infection. If you are undergoing medical treatment, the dentist may also coordinate care with your treating doctor to ensure safe recovery.
Book Your Appointment for Oral Mucositis or Mouth Sores Treatment in Hyderabad Now!
If mouth sores, burning, or pain are improving, continue the daily care routine and monitor closely. If pain does not settle, eating or drinking becomes difficult, or sores keep spreading, a dental check is the right next step. Early evaluation helps confirm whether the problem is oral mucositis or another cause and prevents infection or treatment delays.
At National Dental Care, the best dental hospital in Hyderabad and dental clinic in Hyderabad, our dentists assess mouth sores carefully and guide you with the right treatment plan. This includes identifying local triggers, managing pain safely, and coordinating care when medical treatment is involved.
Whether you’re looking for a dental clinic near me, the best dental clinic in Bangalore or the best dental hospital in Bangalore, National Dental Care offers all the dental treatments. Call our experts now at +91 91692 69369 to book your appointment.
Frequently Asked Questions
What are the most common oral mucositis symptoms?
Common oral mucositis symptoms include burning, soreness, redness, and painful ulcers. Eating and swallowing may become difficult.
What are the main oral mucositis causes?
Oral mucositis causes often include chemotherapy, radiotherapy, head and neck radiation, and local irritation such as sharp teeth or infections.
What is the safest oral mucositis treatment at home?
Gentle brushing, bland rinses, keeping the mouth moist, and avoiding irritating foods are safe first steps. Worsening pain or fever needs professional care.
When should a dentist be consulted for mouth sores?
Dental care is needed when sores spread, pain increases, or food and fluid intake drops.
Can oral mucositis lead to infection?
Yes. Open sores can increase infection risk, especially when immunity is low. Fever, pus, or heavy bleeding needs urgent attention.

 FAQs
FAQs Send us a Message!
Send us a Message!